Does a vegan diet alleviate the agony of rheumatoid arthritis? And even more controversially, does an animal-based diet promote this painful disease? Juliet Gellatley BSc, Dip CNM, founder of Viva! and nutritional therapist investigates and shares a fascinating case study.Never mind text books: what does rheumatoid arthritis (‘RA’) really feel like? I found out through the Healing Well arthritis forum:
I feel like I’ve been run over by a cement roller on my ‘normal’ bad days. On my really bad days I feel like the inflamed joint is literally burning. – Indigo
The pain is extensive, often excruciating… movement is often impossible, although non-movement makes it worse. Do you know what it feels like to get a kink in your neck? Imagine what it would be like to be unable to get rid of that kink. To be unable to move your neck to get rid of the pain or ease the muscles. That is arthritis in a nutshell. Except that it can be anywhere… spine, neck, hips. – IpsoSadly in the UK, around 10 million people have arthritis. Most have the common ‘wear and tear’ form called osteoarthritis but about half a million have the more severe RA. The latter strikes people mainly between the ages of 35 and 50. It is an autoimmune disease in which the body’s defence mechanisms go into action when there’s no threat. The body’s immune system attacks and destroys the affected joints, causing pain and swelling. This can lead to a reduction in movement and the breakdown of bone and cartilage. RA is usually seen in the peripheral joints – especially the hands, elbows, knees and sometimes the feet. It is systemic, so the distribution is usually symmetrical. If you have it on your right side, you usually have it on the left side, too, in the same joints. You have probably seen someone who has swollen and misshapen joints that do not bend properly. These severe changes are often the result of RA.
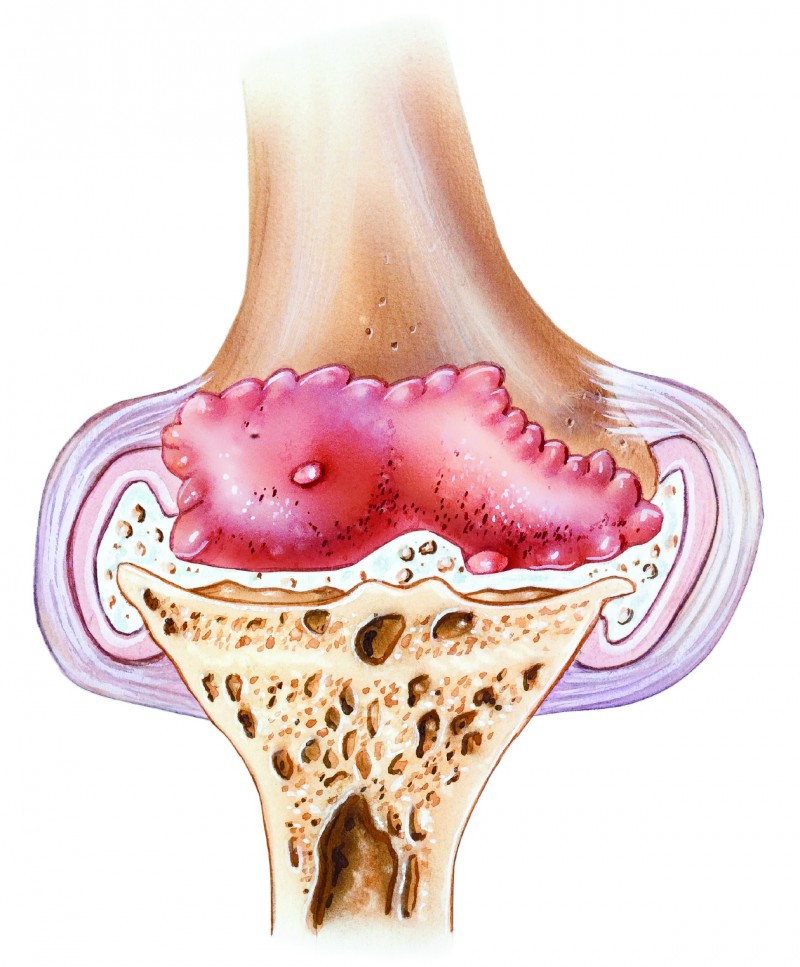
Diet can play an additional role in antigen/antibody problems if a person’s intestines allow large food proteins to enter the body. When we eat, our digestive system breaks the food down into smaller and smaller particles. In most people the particles have to be very, very small – down to their basic components – before they can get from the digestive tract into the body proper. But in some people, proteins are able to get through at an earlier stage, when they are still quite large and complex. This process is called ‘gut leakage.’
When these larger proteins get into the body, they are perceived as antigens (foreign invaders). The body starts attacking them and trying to eliminate them. Eating a high-protein diet, especially one containing animal products, may make people who have a genetic tendency to allow larger particles into their bodies more susceptible to arthritis.Another way that dairy may trigger some people to develop RA is called molecular mimicry. Scientists have found that some people with RA redirect their antibodies, which were meant to fight an unwanted protein, to attack their own joint tissues, which look like the invader. A protein particle of cows’ milk (bovine albumin) is the same as that found in human joints. Pain plummets on vegan diet Unfortunately, arthritis of all types has a poor prognosis under medical treatment. There is no cure for any of the types of arthritis, and medical treatment consists mainly of attempting to relieve pain. New attitudes and behaviors toward arthritis can lead to the lessening, and sometimes the elimination, of pain. The TrueNorth Health Center sees many people experience a decrease in their osteo- and rheumatoid arthritis symptoms after changing their diets. The dietary changes do not reverse the joint deformities, which remain unchanged. But the pain still diminishes, because the improved diet helps reduce the inflammation in the joints. The number of people who benefit from a change in diet varies depending on the research you read. Food sensitivities show up in 20 to 60% of people with RA. Vegan diets assist – and sometimes massively benefit – a staggering half of people with arthritis. There are several important studies that examine the impact of a vegan diet on pain in RA patients. For example, Dr John McDougall et al of St Helena Hospital, California, USA gave 24 meat and dairy consumers with moderate to severe RA a very low fat, vegan diet for 4 weeks. The diet based around common starches such as beans, breads, corn, pasta, potatoes, sweet potatoes and rice. To this centrepiece was added fresh or frozen fruits and vegetables. Participants were encouraged to eat as much as they desired. A rheumatologist who was blind to the study measured RA symptoms before and after the study. The results are remarkable. The degree of pain dramatically reduced; limitation in ability to function improved, joint tenderness and joint swelling significantly decreased. The severity of morning stiffness improved – the only thing not to improve was the duration of the morning stiffness. Vegan diets work because they reduce the exposure of the gut to foods that cause gut permeability. They are very high in antioxidants such as beta carotene, which sits in the cells lining the joint waiting to knock out damaging free radicals. They also contain no red meat, which contains agents that cause inflammation. It is very important that the vegan diet is very low in overall fat but contains fats high in essential fatty acids such as borage oil, evening primrose oil and flaxseed oil because these vigorously fight inflammation. Dietary surveys of people with arthritis revealed that the foods most commonly believed to worsen the condition are dairy products, corn, red and white meats, fish, wheat, eggs, citrus fruits, potatoes, tomatoes, coffee, nuts and bananas. Once the offending food is eliminated completely, improvement usually comes within a few weeks. Dairy foods are one of the principal offenders, and the problem is the dairy protein, rather than the fat, so skimmed products are as much a problem as whole milk. Diet is not the only factor to cause and exacerbate RA, nor is a vegan diet the only way to reduce or eliminate the agony spawned from this disease. But research demonstrates time and time again that a low fat vegan diet is a powerful and positive, drug free and cheap way of limiting the dreadful damage of this disease. Case study In 2012, Carol Coney, 58, of Lincoln consulted me because she had suffered from RA for 14 years. She had been a vegetarian for over 20 years and was almost vegan. Carol believed that the RA was triggered by severe stress. Carol suffered pain, swelling and stiffness of her joints and had some joint deformation. She couldn’t walk without discomfort or pain because her feet were damaged by the disease. I advised Carol to follow a 4-week anti-arthritis diet, which involves eating pain-safe foods such as brown rice, certain cooked or dried fruits, cooked vegetables, essential fatty acids (eg ground flax seed) and plenty of still water (and small amounts of any other foods not on the worst offenders list). At the same time I advised her to avoid the known worst offenders for encouraging inflammation of the joints: all dairy products, corn, meat/fish (not a problem in her case!), wheat and all wheat products, eggs, citrus fruits, potatoes, tomatoes, nuts, coffee and bananas. I also suggested Carol have a half to one teaspoon of powdered ginger daily because of its astonishing anti-inflammatory powers. After 4 weeks, as Carol’s symptoms improved dramatically, I asked her to find out which foods triggered her RA. To do this, she reintroduced the foods that she had eliminated, starting with the least likely trigger, every 2 days to see whether any of her symptoms flared up. Carol was the perfect client, meticulously doing everything asked of her. She reintroduced foods such as tomatoes and potatoes but found she didn’t feel as good as when she was on the anti-arthritis diet and so she returned to it. Carol was excited to tell me of her extraordinary and swift progress:
It is like a miracle. I can walk normally! The general gnawing pain I felt with the arthritis is not there. I am no longer taking any pain killers or anti-inflammatories, except the anti-arthritis drugs given by the hospital.The most gratifying words I’ve heard in a long time were:
I haven’t felt this good in 14 years. My pain-safe vegan diet has given me back my life.

Categories:
Nutritional Advice